HCQ for COVID-19: real-time meta analysis of 414 studies
414 HCQ COVID-19 controlled studies. 66% improvement for early treatment, p < 0.0001. 22% improvement for late treatment, p < 0.0001.
The extreme politicization of HCQ means we must evaluate the data directly.
With 409 controlled studies, 59 RCTs, and extensive supporting evidence, few people have the time and experience to analyze all or most of the evidence. We can reduce the volume by disregarding late treatment studies, however that still leaves 139 studies.
One quick way to confirm efficacy is via prophylaxis RCTs. In the US HERO-HCQ RCT, authors note that combining the US HERO-HCQ and COVID PREP RCTs shows statistically significant efficacy for prophylaxis: "The HERO-HCQ and COVID PREP studies are compared in Supplemental Table 3. Pooling the main results using the Mantel–Haenszel method resulted in an estimate of the common odds ratio of 0.74 (95% CI 0.55 to 1.00) with a p-value of 0.046" Naggie.
A 2022 meta analysis of 7 RCTs by Harvard researchers confirms efficacy for prophylaxis García-Albéniz, as does a meta analysis of 20 studies on HCQ use with rheumatic disease patients Landsteiner de Sampaio Amêndola, along with our analysis of RCTs, and of all PrEP studies. All of these analyses produce similar results.
Some researchers claim that reaching in vitro effective concentrations is not feasible, however direct measurement in treated patients shows that this is false Chaudhary, Ruiz. Notably, the achieved concentrations were highly variable between people, suggesting that not all people may benefit from the same dose.
Like many other treatments, HCQ is effective. The only questions are how effective, under what conditions, what is the optimal combination of treatments, what is the best dosage and treatment regimen, etc.? For these answers, we need to analyze much more of the research.
HCQ reduces risk for COVID-19 with very high confidence for mortality, hospitalization, cases, viral clearance, and in pooled analysis, however increased risk is seen with very low confidence for ventilation.
We show traditional outcome specific analyses and combined evidence from all studies, incorporating treatment delay, a primary confounding factor in COVID-19 studies.
Real-time updates and corrections, transparent analysis with all results in the same format, consistent protocol for 56 treatments.
An analysis of dozens of studies on Hydroxychloroquine and COVID-19 reveals a 72% lower mortality risk when taken early, and a 41% lower mortality risk when given early into hospitalization (when both HCQ and Ivermectin are known to be less effective vs. at first symptoms).

HCQ for COVID-19: real-time meta analysis of 414 studies
414 HCQ COVID-19 controlled studies. 66% improvement for early treatment, p < 0.0001. 22% improvement for late treatment, p < 0.0001.
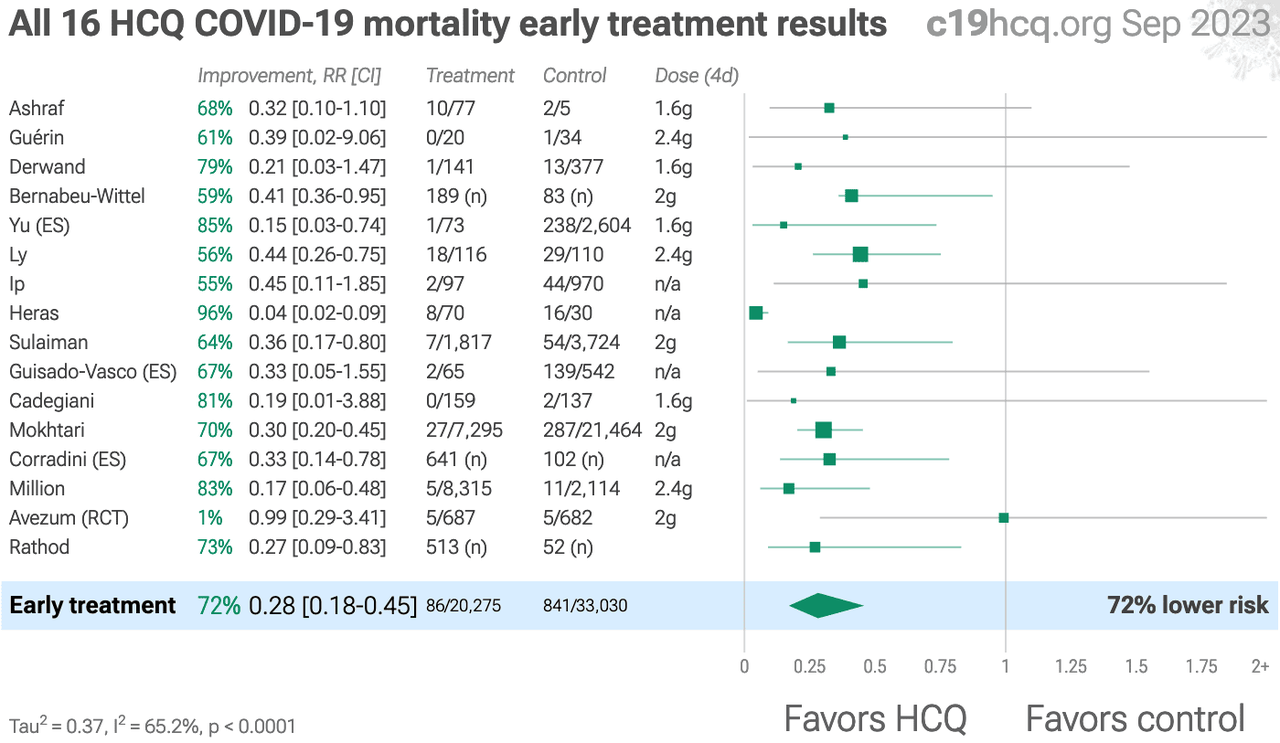
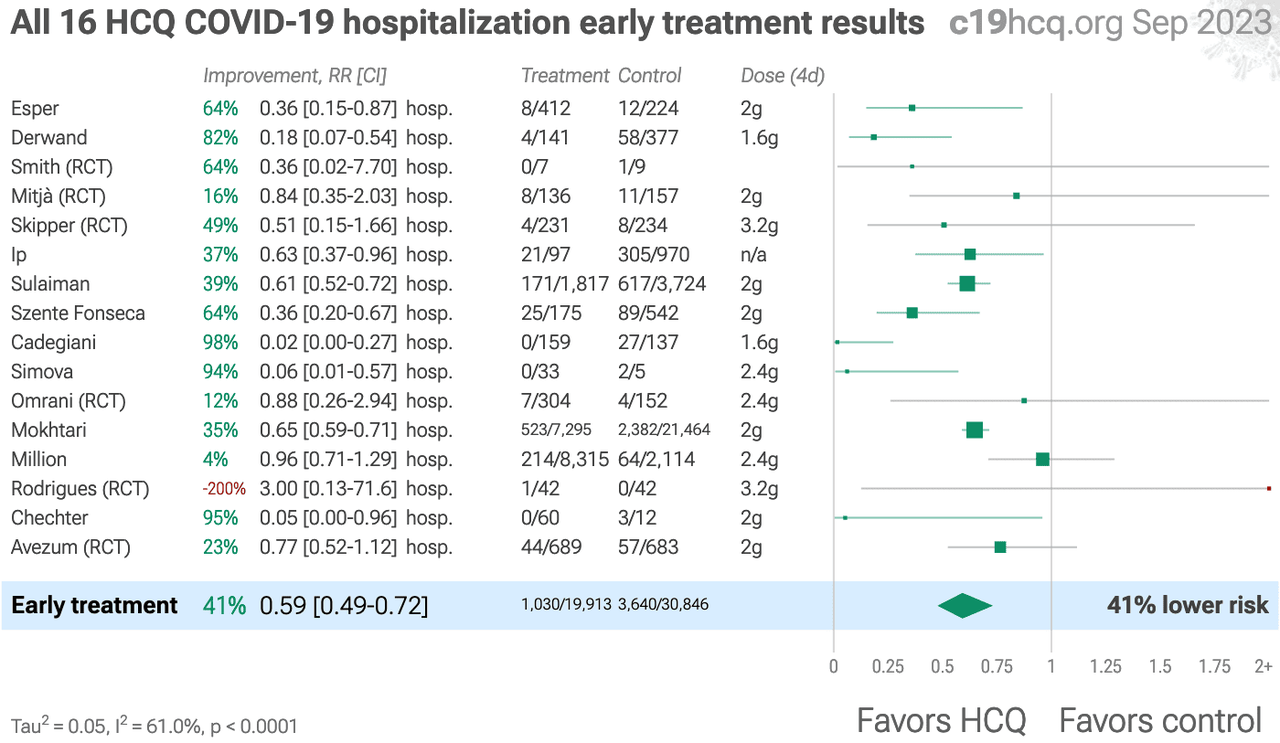
See the full study results here...

HCQ for COVID-19: real-time meta analysis of 414 studies
414 HCQ COVID-19 controlled studies. 66% improvement for early treatment, p < 0.0001. 22% improvement for late treatment, p < 0.0001.
Last edited: